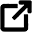
As a dental hygienist, I see many patients who have epilepsy, both controlled and uncontrolled. While epilepsy is a serious neurological health condition, it can significantly impact the mouth and oral health.
Epilepsy can cause people to bite and injure the soft tissues in their mouth, crack or fracture teeth and cause TMJ tenderness and clicking through seizure activity. Antiepileptic drugs can cause dry mouth, gingival overgrowth, and tongue inflammation and contribute to gingivitis development.
In this post, I further expand on the oral effects of epilepsy, how medication plays a role, and tips on protecting teeth from seizures.
Oral health impacts from epilepsy
In the dental office where I work, we see many patients with severe medical conditions, including epilepsy.
It is essential to educate patients who have epilepsy or care for someone with epilepsy to understand the implications it can have on the mouth.
Lip and cheek biting is the most common injury in epileptic patients, with 74%. Tongue injuries occur in about 56% of epileptic patients.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4037794/
When these soft-tissue injuries occur, there is always a chance that an infection or sores can form.
Keeping an eye on the mouth’s tissues after a seizure is essential so dental care and intervention can happen quickly if any issues arise.
But issues don’t just happen to the soft tissues in the mouth. The teeth can be affected as well!
Below is a link to a study of the oral side effects of antiepileptic drugs in children.
Can epilepsy cause teeth problems?
During epileptic seizures, muscles can spasm, contract, and relax, impacting the mouth muscles.
This can make the teeth clench and grind together, and the force can cause wear and tear on the teeth.
Cracks, fractures, chips and tooth wear can all occur from traumatic biting forces caused by seizures.
This damage to the teeth can cause pain, issues with the bite and occlusion (how teeth come together), lead to aesthetic issues and even cause tooth loss. If teeth are too cracked or damaged, it can make the tooth unsavable, and it will need to be extracted.
Epilepsy itself does not cause teeth problems; instead, it is the seizures that can cause the issues and the medication used to treat epilepsy! Below I explain the effects of antiepileptic drugs on the mouth.
How does epilepsy medication affect oral health?
Antiepileptic drugs, also called AEDs, can cause dry mouth, which can cause many dental issues.
Dry mouth, gingival overgrowth, inflammation of the tongue (glossitis), oral thrush, and gingivitis are all side effects of medication used for epilepsy. These effects can impact oral health and should be monitored and treated by a dental professional.
1. Dry mouth
Dry mouth increases the risk of;
- tooth decay
- bad breath
- sore throat
- tonsil stone formation
- gum disease; gingivitis and periodontitis
- increased plaque formation
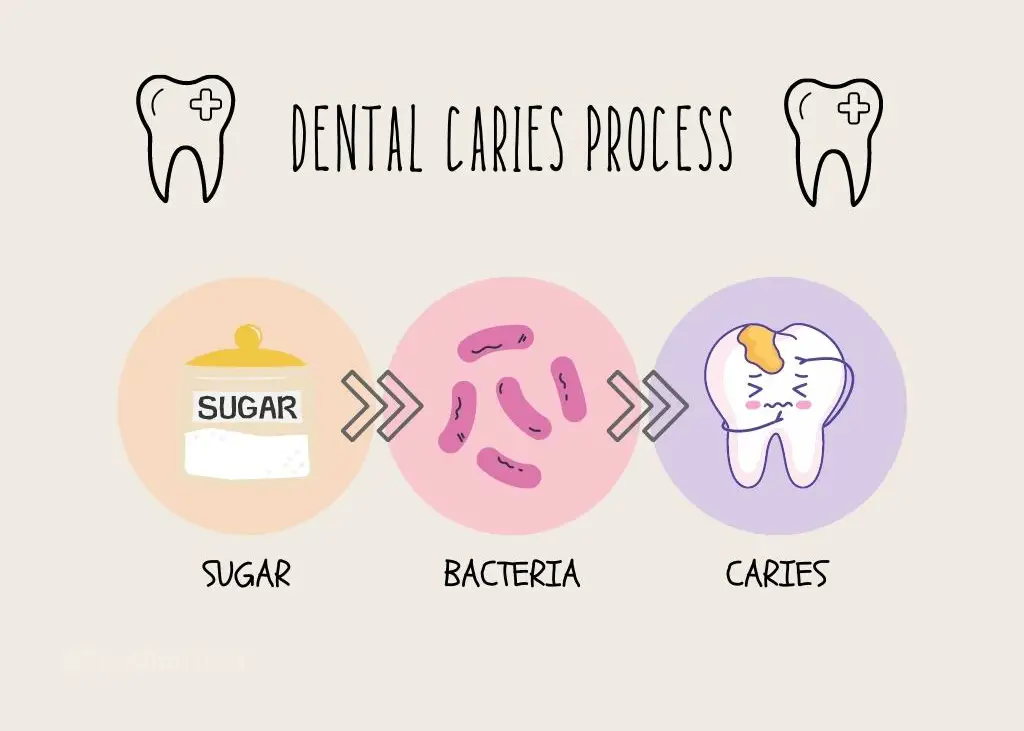
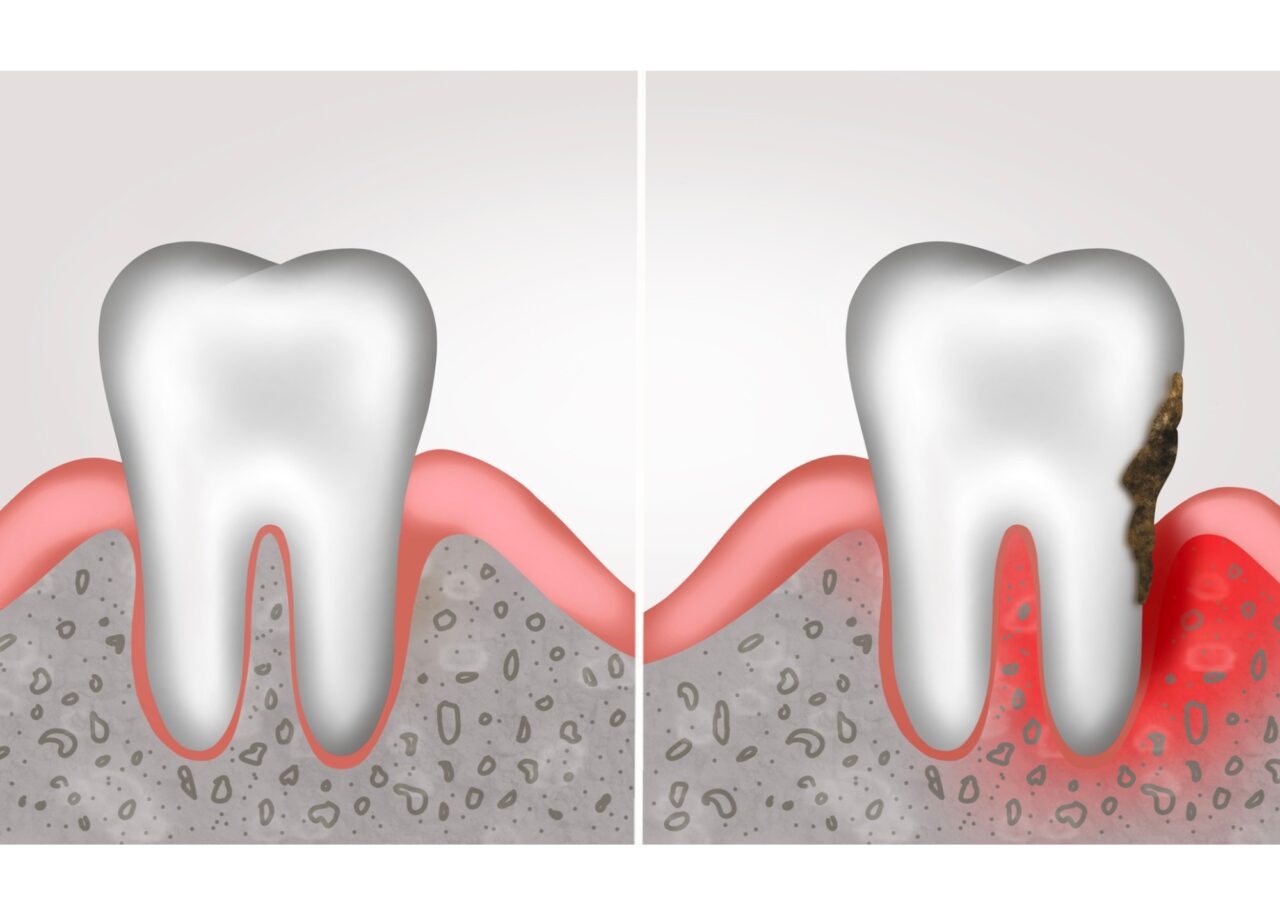
When the mouth is dry, there is not enough saliva to help rinse away food debris and acid that the bacteria produce in the mouth.
The bacteria in the mouth start to consume the sugar from the left behind food, create acid, and multiply rapidly, escalating the number of bacteria in the mouth very quickly.
When the acid is not neutralized, the mouth becomes more acidic, and cavities can form.
If you are worried about dry mouth, I wrote a post that is linked below about how to combat dry mouth and prevent all the oral issues that can arise from dry mouth.
Read Now: How Can I Protect My Teeth From Dry Mouth? 18 Ways
2. Gingival overgrowth
AEDs can also cause gum tissue to enlarge and overgrow. Gum tissue overgrowth is also called gingival hyperplasia.
The gums will have a bulbous appearance and grow downward towards the biting surface of the teeth. This can make the teeth appear shorter and increase the amount of food stuck under the gumline.
Gingival overgrowth can have symptoms of;
- enlarges, bulbous tissue
- inflammation/redness
- discomfort/pain
- increased risk of gum disease
- bad breath
- increased plaque and calculus formation
Having gums that are enlarged can make oral hygiene more difficult. I always recommend to my patients to floss, brush, use a Waterpik, and incorporate warm salt water rinses (if not on a salt-restricted diet).
Read Now: Salt Water Mouth Rinse Recipe for Surgery, Ulcers, Infections
3. Glossitis
Glossitis is inflammation of the tongue. The tongue will appear swollen and could be more red in colour. The tongue may also have a smooth appearance, be tender to touch, and have lesions appear.
4. Oral thrush
AEDs can increase the risk of oral thrush, an overgrowth of yeast in the mouth.
Oral thrush has symptoms of;
- red, inflamed soft tissue in the mouth and throat
- may have a white coating on soft tissues that can be wiped off
- tissue cracking on the corner of the lips
- burning feeling in mouth and tongue
- changes in taste or loss of taste
- cotton feeling in the mouth
5. Gingivitis
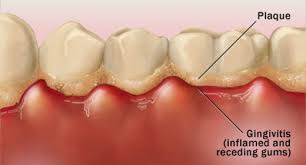
Gingivitis is inflammation that strictly affects the gum tissue in the mouth. Gingivitis is the first stage of gum disease and can lead to tissue death, resulting in bone loss and affecting the body’s overall health.
Please see a dental hygienist regularly to have your teeth cleaned and oral health assessed!
How to protect teeth from seizures
You never want to put something in the mouth when someone is having a seizure.
There is conflicting messaging around using a soft washcloth or something in the mouth to help prevent injury. However, this is a myth.
If someone is having a seizure, and you try to put something in the mouth, you can get injured, and the individual having a seizure can also be injured.
It is best to ensure the environment around the individual having a seizure is clear and monitor the person until the seizure has passed.
After the seizure, you can check to ensure the airway is not obstructed and the mouth and teeth have not been injured or damaged.
Some individuals with epilepsy can have seizures at night. My recommendation for this is to wear a professionally made dental nightguard to protect the teeth.
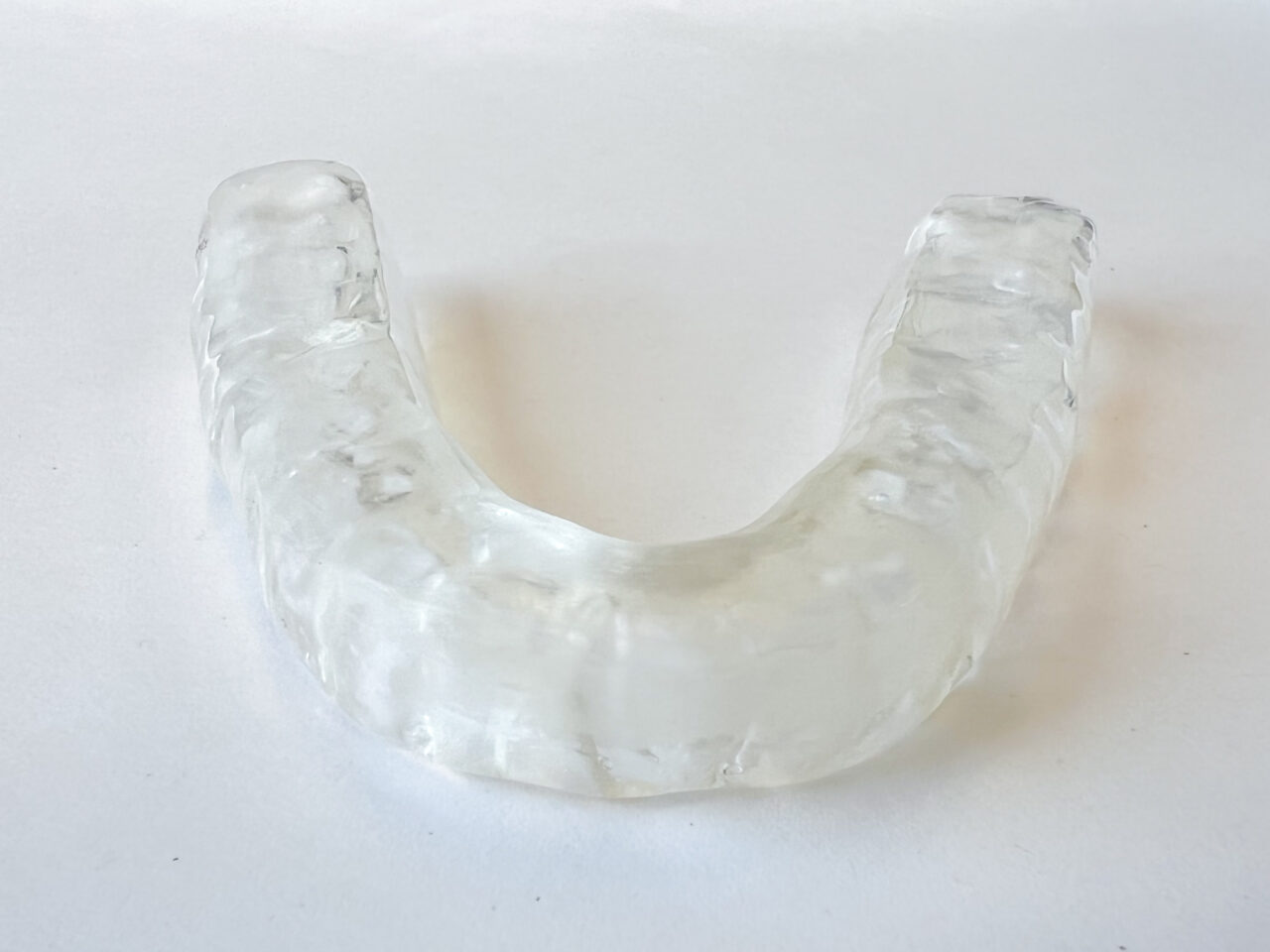
I would not recommend an over-the-counter night guard as it can fit loosely and possibly be a choking hazard.
A professionally made night guard should “click” in and not be able to be removed by the tongue or come off on its own.
Read Now: Can Nightguards Damage Teeth and Bite? Hygienist Explains
Speak with your dental professional about your oral health needs if you have epilepsy, and make sure to disclose that you have epilepsy to your dental professional.
Again, as a dental hygienist, understanding the connection between epilepsy and oral health is crucial to provide the best care to patients.
Holly 🙂