As a dental hygienist, I always ask my patients how many times a week they are flossing. And I get quite a few answers back saying never. I am appreciative of the honesty. However, what happens if you never floss?
If you never floss, you miss cleaning approximately 35% of the tooth surface, leaving it susceptible to accumulating more plaque and calculus (tartar). Along with the body’s immune response, and medical conditions, lack of flossing can increase bacteria, tooth decay, and gum disease.
I will never get angry or upset with my patients who do not floss. Everyone knows that flossing can improve oral health.
I think lecturing people about something they know they should be doing can be detrimental to both trust and respect between hygienists and patients. It can discourage patients from regularly attending dental appointments because it can make them feel belittled.
My way of motivating my patients to floss is to inform them of evidence-based science and explain the potential ill-effects of not flossing.
Below I go over all the evidence-based science for what happens if you never floss. I also include gum disease’s genetic, environmental and bacterial etiology because flossing is not the only factor in gum disease progression. Proper flossing techniques and explaining if it is ever too late to start flossing are also discussed.
What happens if you never floss? Evidence-based science included
Flossing is very effective at removing food debris and preventing calculus formation. As I previously mentioned, if you do not floss, you miss 35% of the tooth’s surface.
Read now: Plackers vs String Floss: Do Picks Work as Well as String?
I have seen improvements in oral health when a patient goes from never flossing to flossing daily. And they can feel the difference as well, with less gum sensitivity and bleeding.
Because flossing disrupts and removes the bacteria and food debris on the teeth and under the gums, it prevents calculus (tartar) formation. Calculus is a calcified mass of bacteria and food debris with a rough texture that cannot be removed at home and will attract more bacteria to attach to the rough surface.
By flossing regularly and preventing calculus formation, you inadvertently break the bacteria accumulating cycle.
Neglecting oral hygiene can directly affect the health of the gums, teeth and bone in the mouth and over-accumulation of bacteria and food debris in the mouth can lead to gum disease progressing.
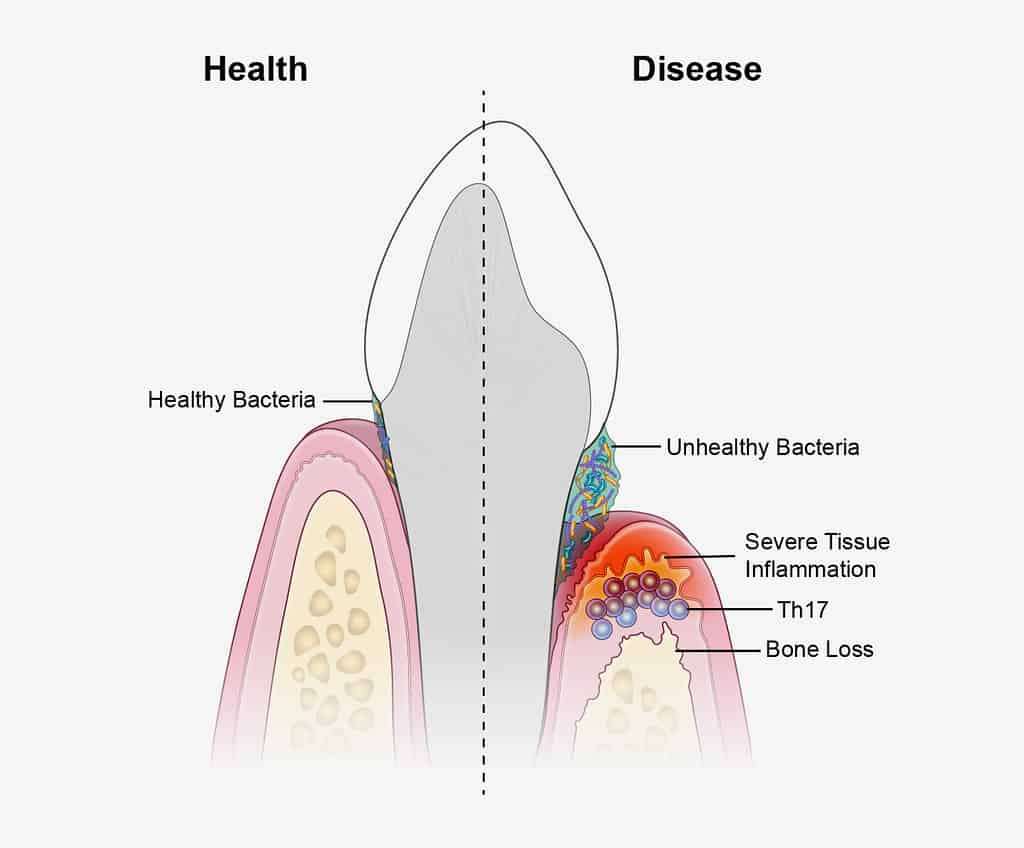
Progression of gum disease; gingivitis to periodontitis
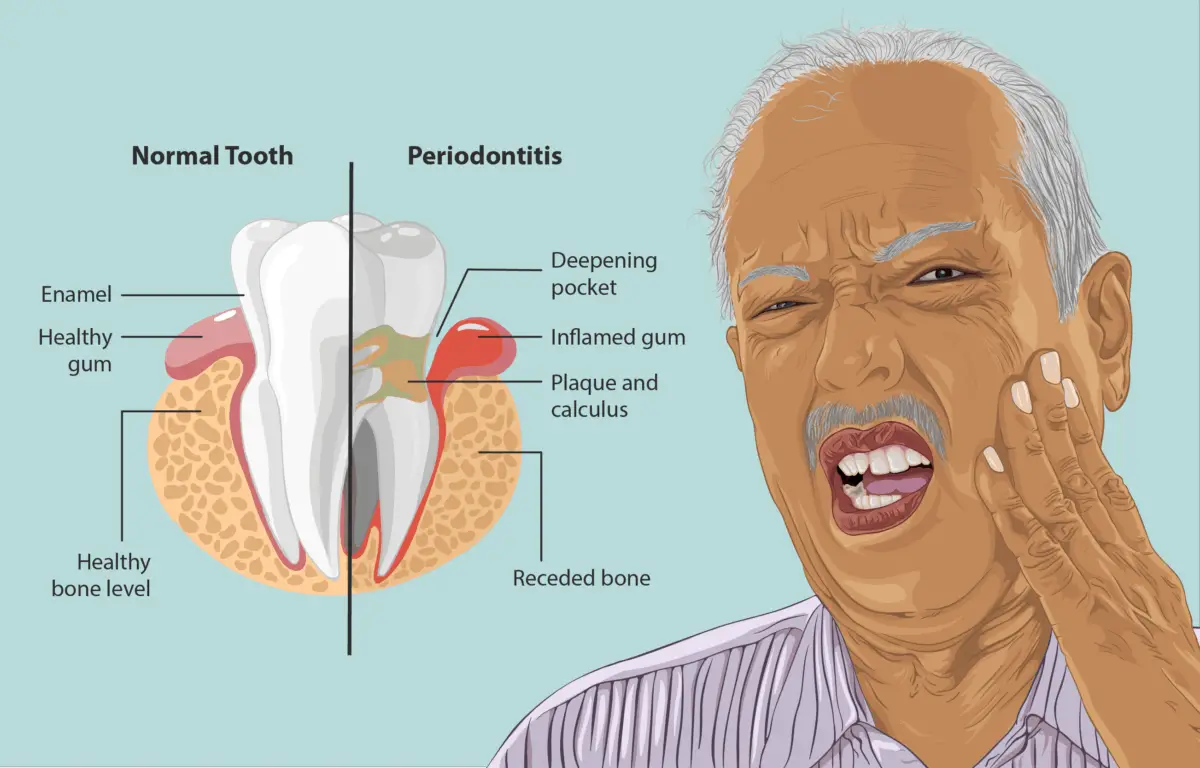
The initial stage of gum disease is gingivitis. Gingivitis is when the infection is isolated to only the gum tissue.
If gingivitis is not controlled and the infection becomes chronic, the disease will progress into the supporting structures of the teeth, including the bone. As you can see in the image above, the right side depicts the progression of gum disease and the human body’s immune response, resulting in bone loss around the teeth and severe inflammation.
When gum disease progresses, the harder it becomes to manage, and the faster gum disease can progress. Advancing gum disease makes it even more critical to have regular dental hygiene appointments to help control the disease and prevent further tissue destruction.
Read now: How Dental Hygienists Clean Teeth! What You Need to Know!
I can’t tell you how many times I have heard an older patient of mine tell me that they regret not taking better care of the mouth because now they have to come to terms with dentures, partial dentures, pain and changes in their face structure due to losing teeth and bone loss.
Flossing plus toothbrushing showed a statistically significant benefit compared to toothbrushing in reducing gingivitis
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6478368/
However, it’s not all about flossing and brushing. There are other aspects to consider.
Gum disease is so multifactorial, and so many medical conditions can be associated with gum disease they are;
- Cardiovascular disease
- Adverse pregnancy outcomes, including premature low birth weight babies
- Respiratory disease
- Chronic kidney disease
- Rheumatoid arthritis
- Obesity
- Cognitive impairment
- Osteoporosis
- Inflammatory bowel disease
- Some cancers
If floss is not an option, using another oral hygiene aid is essential, and sometimes floss is not the best tool for the job. Interdental brushes can be more effective and efficient at disrupting the bacteria in the mouth.
Sometimes dexterity may be a problem for some people, and they may need to use another dental aid such as interdental brushes , GUM soft picks
, GUM soft picks , or a Waterpik
, or a Waterpik . I linked each product on Amazon if you are interested in trying other products than floss.
. I linked each product on Amazon if you are interested in trying other products than floss.
There are other options for people who hate to floss and never will! I would rather my patients use something than nothing. And to be honest, in some situations, these other tools I mentioned can perform better than floss.
Read now: Can Dental Floss Damage Teeth? Hygienist Explains!
Genetic, environmental and bacterial etiology
Not all dental professionals will tell you that some people genuinely don’t need to floss. Some patients brush their teeth once daily, never floss, and their mouth is pristine.
This is extremely rare, and even for my few patients that can carry on a healthy mouth even when they are regularly not flossing, I still recommend flossing at least 3-4 times a week. I still recommend this because gum disease is a silent disease.
Gum disease most often causes no pain and goes unnoticed by the patient for a long time. And you just don’t know when it can start. Preventing gum disease is the best form of treatment.
Unfortunately, there is another group of people who are the opposite. People brush twice a day and floss daily, but their gum disease and bone loss progress rapidly.
Genetic factors for gum disease
33 to 39% of the risk for periodontal disease is related to genetic factors. Source .
.
Genetics determine many factors in our mouth, including;
- tooth structure
- tooth alignment
- immune response
- saliva composition
- mental illness that impedes the ability to maintain oral hygiene routines
- genetic mutations of teeth (incompletely formed teeth, lack of calcification of teeth)
- age of the patient
Genetic disorders and medical conditions are also associated with an increased risk of gum disease. These genetic disorders and medical conditions include;
- Down syndrome (Trisomy 21)
- Chediak-Higashi syndrome
- Papillon-Lefèvre syndrome
- Ehlers–Danlos syndrome
- Hypophosphatasia
- Osteoporosis
- Blood disorders
Environmental factors for gum disease
If you wanted more information, I linked this study to the environmental and other modifying factors of periodontal disease.
to the environmental and other modifying factors of periodontal disease.
- smoking
- vaping
- chewing tobacco
- nicotine pouches
- stress
- socioeconomic status
- HIV infection
- immunosuppression
- sex hormones (especially during pregnancy)
- medications
Bacterial factors for gum disease
We have over 500 species of bacteria in our mouths, and with genetic and environmental factors, the bacteria can begin to wreak havoc on the mouth. As I mentioned in this post, the bacteria will accumulate in the mouth if not disrupted by flossing and brushing.
Once the amount of bacteria reaches a certain amount, certain bacteria begin to thrive (gram-negative bacteria) and release endotoxins that can initiate the immune response and cause gum disease.
Not all the bacteria in our mouths are harmful. We need bacteria to live healthy lives. But too much is not good, providing the foundations for infections.
Through flossing and brushing, the amount of bacteria is reduced and prevents endotoxins from infiltrating the gums and supporting structures of the teeth and the bloodstream.
Once the bacteria enters the bloodstream, it travels around the body, increasing the risk of other medical conditions, including heart disease.
After researchers adjusted for factors like age, gender and smoking, they found that people who flossed once or more each week were 17% less likely to have gum disease than those who flossed less frequently.
https://www.jnj.com/health-and-wellness/benefits-of-flossing-gum-disease-prevention
Flossing and its role in preventing heart disease
Gum disease has not been proven to cause these medical conditions, but the association is clear.
A new emerging science explores the concept that gum disease is more of an autoimmune disease, and some people are genetically predisposed to the condition. Source.
Our oral health is linked to our entire body’s health, and doing everything we can by flossing regularly can help prevent heart disease.
Can gingivitis be cured? Dental hygienist explains
Gingivitis can be reversed, but periodontitis can not be. Gingivitis is inflammation of only the gum tissue surrounding the teeth. Once inflammation extends further into the gum tissue and the bone surrounding the teeth, as seen in periodontitis, gum tissue and bone tissue can be permanently lost.

Proper flossing technique; C-shape flossing
Flossing with proper technique can ensure that the teeth’ critical surfaces are not missed and avoid injury to the gum tissue.
If flossing is done incorrectly, with too much pressure, it can lacerate the gum tissue, causing clefting and gum recession.
The best way to floss is by using string floss and wrapping it around the tooth in a C-shape
When the floss is wrapped around the tooth as much as possible in a c-shape, it covers more surface area of the tooth and will go further under the gumline safely.
Read now: How to Use String Floss; Steps of Use With Pictures
Is it too late to start flossing? Hygienist explains!
It is never too late to start flossing, regardless of age or oral health status. Flossing helps prevent inflammation, bone loss, and tooth decay. Flossing promotes oral and overall health because it helps clear away bacteria that can enter the bloodstream and travel throughout the body.
I have seen so many older patients who have impeccable dental hygiene that they wish they had started earlier to prevent their gum disease. They started flossing and cleaning their teeth and gums later in life.
However, what I tell them is at least they started late than never, and they are doing everything they can to slow down and prevent the gum disease from progressing.
Every little bit counts, and I want to encourage my patients to continue their hard work, becuase it does pay off!
I hope you have found the information I have given you helpful!
Have a wonderful day,
Holly 🙂

